By Michael O’Brien
The Athens (Ohio) News, Sept. 22, 2013
At a recent public forum, community members had the opportunity to learn more about single-payer health-care systems.
The forum was hosted by the Single Payer Action Network, Ohio (SPAN), a statewide coalition of organizations and individuals who say they’re working to enact fundamental health-care reform that guarantees full and comprehensive access to a full range of medical services.
Insurance exchanges under the Patient Protection and Affordable Care Act (PPACA) are set to open Oct. 1 nationwide, making access to affordable health care a primary concern for many Ohioans.
Whether referred to as single-payer or Medicare for all, SPAN believes the current market-driven system is not sustainable. Under a single-payer health-care system like Medicare, medical service providers would be paid directly by the federal government.
During an opening presentation, SPAN Ohio Director Debbie Silverstein stressed that the issue of health care and the Patient Protection and Affordable Care Act evokes very strong emotions.
“We want health care to be there when we need it but what if resources aren’t there? Obamacare is a good start but we’re not done yet,” Silverstein said. “Health care is a basic human need.”
Proponents of single-payer systems cite reduced administrative costs in Medicare compared to those of for-profit medical insurance companies. Silverstein noted that since 1970, the health-insurance industry has seen a 2,500 percent rise in the number of administrative jobs compared to a roughly 100 percent increase in jobs for direct health-care providers.
Opponents to single-payer systems argue that Americans without health insurance are not denied access to care, citing federal law that requires hospitals to treat people without insurance.
Speaking in Cleveland in 2007, then-President George W. Bush addressed an effort in Congress to expand eligibility to State Children’s Health Insurance Program (SCHIP), cited a common argument against government having a larger role in access to health care.
“I mean, people have access to health care in America. After all, you just go to an emergency room,” Bush said. “I mean, think of it this way: They’re going to increase the number of folks eligible through SCHIP; some want to lower the age for Medicare… to get more people to be a part of a federalization of health care. In my judgment, it would lead to not better medicine, but worse medicine. It would lead to not more innovation, but less innovation.”
Silverstein used her own experiences to illustrate the difference between medical services in the U.S. and France, which provides universal health care.
While visiting a sister in France, Silverstein said she suffered a severe foot injury, the result of tripping on a curb. Despite her concern over the cost, Silverstein went to an emergency room at a Paris hospital.
“I was afraid I had broken my left foot,” she recalled. “After some deliberation due to concern for cost, I did go to the emergency room. When I explained that I had fallen, the first question asked was ‘Madame, when you fell, did you hit your head?’ They then proceeded to evaluate my problem and get me checked in. My bill for the emergency room visit was zero.”
Silverstein explained that her experience at an Ohio hospital was very different and illustrative of what many Americans experience when seeking medical care. Suffering from severe headaches, Silverstein sought care at a Cleveland hospital.
“I suffered a very bad headache that was unrelenting unless I was flat on my back,” she said. “After six weeks, a friend suggested I try the Headache Clinic at the Cleveland Clinic. I called to make an appointment and started to explain my symptoms. I was interrupted and was asked if I had insurance. I had to go through the insurance verification before they were concerned about my condition.”
The event’s panel discussion included Silverstein, Ohio University professor of sociology Deborah Thorne and local health-care advocate Warren Hayden. All agreed that the negative economic impacts of medical debt are widespread even for people with insurance.
Thorne stressed that even the rich are not immune to the consequences of getting sick in American. In 2008, Thorne coauthored a book with now Massachusetts Sen. Elizabeth Warren titled “Get Sick, Go Broke. Health at Risk: America’s Ailing Health System-and How to Heal It.”
Thorne said her research into medical bankruptcies shows 62 percent of all personal bankruptcies nationally result from medical debt, and 78 percent of the people involved had insurance at the onset of their illness. A follow-up study, focused on Massachusetts, which has a system similar to the ACA, showed little difference in the percentage of medical bankruptcies.
“Medical debt is a leading factor in 49 percent of home foreclosures, and medical debt is one of the leading reasons middle- and lower-income Americans cannot get financing to purchase a home,” Thorne said. “The PPACA will not necessarily lower incidence of medical bankruptcy. Unless you’re Bill Gates, you are not immune to medical bankruptcy.”
As for the future of health care going forward, beginning in 2017, provisions in the PPACA would grant exemptions to states that develop plans similar to those in the health-care law including single-payer or Medicaid for all systems. SPAN sees this as an opportunity to enact a single-payer system in Ohio.
“Over 60 percent of all health-care costs in the U.S. are paid for by taxes,” said Hayden. “When you look at Medicare, Medicaid, veterans, anyone who works for the government and a number of non-profits funded by the government, there are huge amounts of tax dollars already going into the system. We would not need a whole lot more because of the savings that would come about from a single-payer system.”
SPAN supports on effort by Healthy Ohioans Work to place an initiative on the 2014 ballot that would force the state to expand Medicaid in Ohio and would put the state on the road to a single-payer system. Ohio is one of several states that have opted not to expand Medicaid coverage despite a guarantee of federal funding. Gov. John Kasich has pressed the Republican-controlled Legislature to act but the House and Senate have so far resisted the expansion.
At the close of the forum Silverstein expressed surprise that the audience did not raise the issue of individuals having to pay for someone else’s health care.
“We are all in this together. We are a society, a community, and Americans have always cared about each other and have always cared for one another,” Silverstein said.
http://www.athensnews.com/ohio/article-40672-forum-asks-is-single.html
A Man Who Worked Too Hard
By Andrew D. Coates, M.D., F.A.C.P.
WAMC Northeast Public Radio, Sept. 20, 2013
Influenza rocked our community hospital for weeks last winter just as the first snowstorms came. Our hospital medicine service was swamped with patients. I was working the night shift.
One emergency physician dramatically recounted how a queue of ambulances had clogged the parking lot. Once all of the emergency department beds, hallway spaces, and waiting room seats were taken, patients waited outside in ambulances. With the usual triage system in gridlock, he had climbed into ambulances one by one to help triage or stabilize patients.
Such are the undignified consequences of a system that encourages hospitals to run themselves like factories or just-in-time warehouses.
One patient’s admission stood out.
A young-looking man in his early 40s had keeled over while shoveling snow. As I admitted him to the hospital, National Weather Service advisories that mention the dangers of snow shoveling and warn persons at risk for ischemic heart disease to be cautious (mostly those who are past our chance at preventive medicine) flashed through my mind.
Yet, this person had not been merely shoveling some snow. He had been running a snowblower, as well as manually shoveling, from shortly after 3:00 a.m. until a quarter past 6:00 p.m. – just over 15 hours straight, without a break. I asked what he had eaten. Nothing. He had consumed only about a half gallon of liquids all day. The previous day he had tried to eat a chicken salad sandwich but managed to down only about one third of it because a sore tooth prevented him from eating.
In fact, he had not had much solid food for more than a week.
The patient had an untreated breaking, decayed molar with an adjacent gum abscess. He had no health insurance. Seeing a dentist meant an outlay of cash that he didn’t have. Our patient, able to find steady work only in summer months, had jumped at the chance to earn money during the snowstorm. He concluded his explanation with a stoic shrug, saying that his tooth was beginning to feel better now that part of it had broken off.
I finished taking the patient’s history, performed a full examination, and retreated to review his data in full. His test results were normal. Apart from his dental abscess, he seemed rather healthy. He received no medicines and had no chronic illnesses. Assessment: He had worked himself into the ground – and this wasn’t his fault. He had done what he could to help himself. Unfortunately, he also needed to pay attention to taking enough fluids and food to sustain his exertion. Like an increasing number of our patients, this man was living at the very edge.
From a physiologic point of view, our patient had just had a big all-day-long stress test. His outlook and insight; history of good health; normal vital signs; and normal results on his physical examination, EKG, laboratory values, and head CT all spoke of someone who had passed the test with flying colors. A sick person might have collapsed before dawn, not after sunset, on such a day of work.
As we discussed these findings, I sought to reassure him. When I suggested that perhaps he really didn’t need more tests, he seemed shocked. “We need to get to the bottom of this!” he exclaimed.
In spite of his meager means, he wanted admission to the hospital and the full work-up promised. He mused that he might apply for Medicaid but recognized that if he didn’t qualify, the ambulance and hospitalization might cost thousands of dollars, with bills for years to come.
Once admitted on observation status, our patient found one of the only available beds – in the intensive care unit. He was released the next day after receiving more normal laboratory results.
On reflection, the experience left me feeling less like a doctor and more like a hapless worker bee in a buzzing but somehow misguided hive, fraught with unnecessary and avoidable endeavors.
Moreover, if the patient had access to dental care, he would have been able to take adequate fluids and calories and perhaps never would have collapsed in the first place. Lastly, here was a glimpse of the health consequences of an economy increasingly reliant upon temporary, part-time, and seasonal jobs.
It was redeeming to recognize that I had helped him by initiating treatment for his dental infection. Yet, the experience also reaffirmed my strong belief that our nation needs, at minimum, a public, single-payer program that will provide care – and system planning – for every patient. What good we could do if we mustered, rather than squandered, our resources.
This case of a man who worked too hard illuminated how feeble, even irrelevant, our profession may seem when it comes to basic requirements of personal health in the 21st-century United States. We have earned great scientific and human insight into the lives of our patients. To practice the art and science of medicine, to fulfill the calling of our profession, we must ultimately learn to articulate our insights to guide social resources toward the health of each and all.
If we continue to embrace the role of worker bees, focused upon chart checklists and testing algorithms and petty incentives to generate revenue, we will place ourselves in a role unworthy of our profession.
To eliminate unnecessary tests and treatments – and to prevent so many avoidable illnesses – our profession will need to heal itself.
Dr. Andrew Coates practices internal medicine in upstate New York.
You can listen to Dr. Coates’ radio broadcast here: http://wamc.org/post/man-who-worked-too-hard
Single-payer system would succeed
By Michael C. Huntington, M.D.
Register-Guard (Corvallis, Ore.), Letters, Sept. 9, 2013
In response to a July 31 column about single-payer health care, Reginald Jensen, a retired insurance underwriter, strayed from credibility as he dismissed the ability of single-payer systems to lower costs (“Single-payer system is just too costly to work”).
In doing so he ignored the success of 22 wealthy countries and our own Department of Veterans Affairs, which use single-payer systems to provide better care for more people at far less cost than does the U.S. market-based health care system.
Single-payer can be defined as a type of financing system for health care such that one entity — on behalf of and directed by the public through government or a public/private agency — collects all health care fees and pays out all health care costs. Under such a financing system, health care can be delivered through both private and public providers just as it is now, but with the public setting standards of care and negotiating prices.
Jensen didn’t mention that the United States pays, per capita, twice as much for health care as other countries do and has poorer outcomes by many criteria, according to the Organization for Economic Cooperation and Development and the World Health Organization.
His claims — that European health care costs could surpass U.S. costs, that Europe’s humane health care systems somehow cause economic crises, that we can solve our health care crisis through more jogging or personal discipline, that taking care of all of us means indenturing some of us — are baseless.
Dr. Michael C. Huntington resides in Corvallis.
http://registerguard.com/rg/opinion/30407489-78/care-health-system-quality-eugene.html.csp
What if Medicare covered everybody’s medical care?
By Betty Johnson
Gazette-Times (Corvallis, Ore.), Letters, Sept. 19, 2013
Members of Mid-Valley Health Care Advocates posed this question to area residents at the celebration of Medicare’s 48th birthday party at Riverfront Park this summer: How would your life be different if we had Medicare for all?
Here are some of the thoughtful answers which area residents wrote on notes which they attached to the writer’s wall:
“My granddaughter would not be bankrupt and uninsurable at age 30.”
“I would no longer lay awake every night in abject terror of my future.”
“I’d feel that things were fairer.”
“My husband could take a job that would let him come home every night.”
“As a physician, I would stop worrying about all the people I know who are needlessly suffering with untreated illness.”
“My wife would be covered, and I could retire.”
“My 29-year-old daughter, who is fighting cancer, would not be bankrupt … and I would not, in covering her co-pays, be headed toward bankruptcy.”
“I’d start a business.”
“My friends, family and I could replace our glasses.”
“As a healthcare provider, I could make decisions based on clinical factors, not an individual’s financial (insurance) situation.”
“I’d be living in a country that reflects a sense of community and caring and I would no longer be embarrassed to be an American.”
And the last response sums it up … for me and, I hope, for you … “Health Care for all is the way it should be. Why is it taking us so long?”
Betty Johnson resides in Corvallis.
http://www.gazettetimes.com/news/opinion/mailbag/letter-what-if-medicare-covered-everybody-s-medical-care/article_b71dac94-2107-11e3-a31b-0019bb2963f4.html
Health care coverage for the homeless
Medicaid Expansion: Chronically Homeless Adults Will Need Targeted Enrollment And Access To A Broad Range Of Services
By Jack Tsai, Robert A. Rosenheck, Dennis P. Culhane and Samantha Artiga
Health Affairs, September 2013
Prior to health reform, eligibility for Medicaid was limited to low-income people in certain categories, including children, pregnant women, parents with dependent children, people who qualified as disabled, and elderly adults. The Medicaid expansion in 2014 extends eligibility to low-income, nonelderly, nondisabled adults without dependent children—often called “childless adults”—who were historically excluded from the program.
Among other people who could gain coverage under the Affordable Care Act’s Medicaid expansion are the estimated 1.2 million people across the country who are homeless in a given year, including roughly 110,000 chronically homeless adults. Given their low incomes, many currently uninsured or underinsured homeless adults will gain from the Medicaid expansion a new pathway to coverage and new health care opportunities.
Conclusion
The Medicaid expansion under the Affordable Care Act will likely increase coverage options and provide broader access to care for many chronically homeless adults who are uninsured or rely solely on state or local assistance programs. Moreover, states that expand Medicaid may experience offsetting cost savings, as chronically homeless adults who previously relied on state and local assistance transition to Medicaid. Conversely, in states that do not expand Medicaid coverage, poor uninsured adults will not gain a new coverage option, and many will likely remain uninsured and continue to face barriers to accessing needed care.
The findings of this study illustrate the broad and varied health care needs of chronically homeless adults. Ensuring access to preventive and mental health services is particularly important for addressing the needs of this population, and the services available to this group should include case management and other supportive services, such as help with housing.
http://content.healthaffairs.org/content/32/9/1552.abstract
Comment:
By Don McCanne, M.D. For those states that expand Medicaid, many of the chronically homeless will have an opportunity to obtain health care coverage – much needed in this vulnerable population. However, these individuals face many hurdles in both initial enrollment and maintaining enrollment in Medicaid. Many will still be without adequate coverage. This is unfortunate since we could have eliminated the coverage problem by establishing a single payer national health program – enroll once and it is for life. We could still do that. For more information on health care for the homeless, see the website of National Health Care for the Homeless Council: http://www.nhchc.org
]]>The high costs of complexity in health care reform
By Philip Caper, M.D.
Bangor (Maine) Daily News, Sept. 19, 2013
I have great admiration for the political courage of President Barack Obama and the congressional leaders who were willing to take on health care reform, justifiably called the “third rail” of American politics. Our system cries out for reform. But they made a fatal mistake in allowing the law to be drafted by Congress, which is composed of 535 members with vastly varying values, goals and interests.
Consequently, the resulting law is a conglomeration of ideas from across the political spectrum, thrown together and lacking any coherent conceptual framework. (Congress is usually a better editor than author.) This lack of coherence has resulted in a law that is far too complicated and therefore too expensive to manage, full of holes, will be appliedunevenly and unfairly, be full of unintended consequences, and be easily exploited by those looking to make a quick buck.
It has been credibly estimated that administrative costs make up more than 30 percent of our national health care bill, most of it unnecessary. The waste in this area alone isequivalent to around $400 billion annually. That is more than enough to provide health care to every uninsured person living in our country. Some of these costs result from the slicing and dicing of Americans into ever-tinier and more confusing categories, the inevitable result of applying the principles of insurance to health care.
But the costs go beyond dollars to a lack of basic fairness, and of public understanding and support.
A plurality of the public still views the law negatively. Even many experts are confused by it. The law tries to deal with this confusion by providing a host of federally funded“navigators” to help people find their way through the maze it creates. While this provision will provide many well-paying jobs, it uses health care funds but does not pay for any health care — an example of your health care dollars not at work.
The ways in which the costs and benefits of the law are distributed are patently unfair. Even if it is perfectly implemented, it will leave around 30 million Americans without health care coverage. Some of this was intentional, but some wasn’t. The Affordable Care Act’s architects intended the federal government to expand the Medicaid program and make it more uniform to cover the poorest among us on a fairer basis.
But the Supreme Court found that requiring the states to expand their Medicaid programs would be unconstitutional, thereby gutting that provision. About half the states, including Maine, have declined the Medicaid expansion. They have decided to forgo the 100 percent federal funding (dropping to 90 percent after three years). That has created the anomalous situation where some of the poorest Mainers will receive no help, while those who are slightly wealthier will receive federal subsidies to buy insurance.
Similarly, some people who make too much money to qualify for any federal assistance but cannot afford increasingly expensive health insurance on their own will continue to pay state and federal taxes to finance Medicare, Medicaid, the VA and other programs for others. They will also pay higher federal taxes to compensate for the fact that private insurance for union members, corporate executives, and others with employment-based coverage, some of it quite comprehensive, is tax exempt.
The ACA does not go nearly far enough in restraining ballooning health care costs or reforming the way we pay those providing health care products and services. These abuses have been brilliantly and persuasively documented in Steven Brill’s Time Magazine cover story “ Bitter Pill.” Health care prices are completely out of control and the uninsured, many of them the least able to pay, are often the only ones charged full sticker price.
The only persuasive reason that has been given for our failure to address these glaring problems is that the power of the health care industry (that spends three times as much on lobbying as the defense industry) is too great. Pretty pathetic, and yet another example of your health care dollars at work — this time against you.
It doesn’t have to be this way. It is now well-documented that Medicare, a far simpler program than the ACA, spends much less on administration and is much more effective in controlling prices than private insurance. Apologists for the existing system of private insurance claim that it preserves “choice” of insurers, and that Americans want that choice.
But the choice people really want is a choice of health care providers, not insurance. Medicare beneficiaries can already choose any participating provider they wish. I have never heard a single Medicare patient complain about not having more choice of insurance companies.
Even Sen. Harry Reid, one of the ACA’s architects, now admits that it must be a way-station to a Medicare-like, single-payer plan. He has said he thinks the country has to “work our way past” insurance-based health care.
Fortunately, in Maine we have a couple of ways to do that. Next year, hearings will be held on L.D. 1345, co-sponsored by Rep. Charlie Priest and Sen. Geoff Gratwick. That bill would start us on a path toward a statewide nonprofit, unified and universal health care system, similar to the route recently taken by our neighbors in Vermont.
Failing approval of that measure, Maine (unlike Vermont) has a referendum process, a direct vote of the people for sanity in health care. If we were to follow either path, Maine would once again have the right to say “Dirigo” — I lead — and set a historic example for other states to follow.
Physician Philip Caper of Brooklin is a founding board member of Maine AllCare, a nonpartisan, nonprofit group committed to making health care in Maine universal, accessible and affordable for all. He can be reached at pcpcaper21@gmail.com.
http://bangordailynews.com/2013/09/19/health/the-high-costs-of-complexity-in-health-care-reform/
]]>CMS Office of the Actuary on growth in health expenditures
National Health Expenditure Projections, 2012–22: Slow Growth Until Coverage Expands And Economy Improves
By Gigi A. Cuckler and colleagues in the Office of the Actuary at the Centers for Medicare and Medicaid Services (CMS)
Health Affairs, October 2013
Health spending growth through 2013 is expected to remain slow because of the sluggish economic recovery, continued increases in cost-sharing requirements for the privately insured, and slow growth for public programs. These factors lead to projected growth rates of near 4 percent through 2013. However, improving economic conditions, combined with the coverage expansions in the Affordable Care Act and the aging of the population, drive faster projected growth in health spending in 2014 and beyond. Expected growth for 2014 is 6.1 percent, with an average projected growth of 6.2 percent per year thereafter. Over the 2012–22 period, national health spending is projected to grow at an average annual rate of 5.8 percent.
National Health Expenditures (NHE):
2013 $2.915 trillion
2022 $5.009 trillion
NHE per capita:
2013 $9,216
2022 $14,664
NHE as percent of Gross Domestic Product (GDP):
2013 18.0%
2022 19.9%
2014 Growth Rates By Selected Sector, Before And After The Impact Of The Affordable Care Act
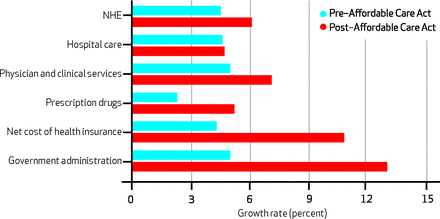 SOURCE: Centers for Medicare and Medicaid Services, Office of the Actuary, National Health Statistics Group.
http://content.healthaffairs.org/content/early/2013/09/13/hlthaff.2013.0721.abstract
Link to bar graph:
SOURCE: Centers for Medicare and Medicaid Services, Office of the Actuary, National Health Statistics Group.
http://content.healthaffairs.org/content/early/2013/09/13/hlthaff.2013.0721.abstract
Link to bar graph:
http://content.healthaffairs.org/content/early/2013/09/13/hlthaff.2013.0721/F2.large.jpg
Comment:
By Don McCanne, M.D. Celebrating the slowing of the rate of increase in health care spending is premature, judging by the conclusions of the experts at the Office of the Actuary at CMS. Over the next decade, health care costs will continue to increase at a rate of about 6 percent annually, reaching nearly 20 percent of our GDP by 2022. If the Affordable Care Act (ACA or Obamacare) will not adequately control health care inflation, then what financial impact is it having? Look at the bar graph above. The differences represent only the impact of ACA in 2014 and not the other economic factors that the actuaries took into consideration in this report. Instead of slowing the growth in our national health expenditures, ACA will increase spending. This is expected because of the numbers of individuals who will gain coverage through the expansion of Medicaid and the establishment of the state Marketplaces (exchanges). Had we enacted single payer reform instead, the savings from the efficiencies would have offset the costs of even greater expanded coverage, including everyone. Most of the increases in coverage will be amongst healthier children and younger adults. For that reason hospital care is not expected to increase much due to ACA, but physician and clinical services and prescription drugs will increase significantly now that these individuals will have more affordable access to health care. The net cost of health insurance (premiums earned minus benefits paid) will skyrocket, since, after all, ACA was a gift to the private insurance industry. Obviously much of that represents an increase in the administrative waste that characterizes our dysfunctional financing system. “Net cost of health insurance is calculated as the difference between calendar year incurred premiums earned and benefits paid for private health insurance. This includes administrative costs and, in some cases, additions to reserves; rate credits and dividends; premium taxes; and plan profits or losses. Also included in this category is the difference between premiums earned and benefits paid for the private health insurance companies that insure the enrollees of the following public programs: Medicare, Medicaid, Children’s Health Insurance Program, and workers’ compensation (health portion only).” But look at the growth in government administration directly due to ACA. Think of the administrative costs of Medicare – under 2 percent of benefits paid. Now look at the rate of increase in administrative costs that are attributable to a complex, fragmented, multi-payer system of financing health care – flaws greatly compounded by ACA. Government administration “includes all administrative costs (federal, state, and local employees’ salaries; contracted employees including fiscal intermediaries; rent and building costs; computer systems and programs; other materials and supplies; and other miscellaneous expenses) associated with insuring individuals enrolled in the following public health insurance programs: Medicare, Medicaid, Children’s Health Insurance Program, Department of Defense, Department of Veterans Affairs, Indian Health Service, workers’ compensation, maternal and child health, vocational rehabilitation, Substance Abuse and Mental Health Services Administration, and other federal programs.” Although the dollar amount that will be spent by the government on health care administration (projected $70.4 billion in 2022) is a bargain compared to the cost of administration in the private sector (net cost of private insurance projected to be $313.2 billion in 2022), these increases nevertheless are representative of the profound administrative waste of the ACA model of reform. Haven’t you readers had enough of this? Why don’t you go out and do something about it?
]]>Gaps in public understanding of Medicare
The Public and the Conflict over Future Medicare Spending
By Robert J. Blendon, Sc.D., and John M. Benson, M.A.
The New England Journal of Medicine, September 12, 2013
Our thesis is that there exists today a wide gap in beliefs between experts on the financial state of Medicare and the public at large. Because of the potential electoral consequences, these differences in perception are likely to have ramifications for policymakers addressing this issue.
There are concerns about Medicare today and current cost-containment efforts. Most respondents see Medicare in some cases already withholding treatments and prescription drugs to save money, including 63% who believe this happens very often or somewhat often. Also, the public sees the bigger problem for Medicare beneficiaries as not getting the health care they need (61%) rather than as receiving unnecessary care (21%). Medicare pays about half the total personal health care expenditures for beneficiaries, but many people are confused about what proportion is paid by Medicare, whether it pays for most of recipients’ bills or substantially less.
When given a dozen possible causes for rising Medicare costs that have been suggested either by experts or in the media, the majority do not identify any one of them as the most important. However, the three most often cited reasons relate to poor management of Medicare by government, fraud and abuse in the health sector, and excessive charges by hospitals. The lowest ranked reason was the cost of new drugs and treatments being offered to seniors.
Although Medicare is popular, it is not seen as better run than private insurance plans, nor is it seen as particularly different from private coverage with respect to quality of care or access to physician care.
The one area of clear support for the future is the growing preference for Medicare Advantage–type private health coverage among persons less than 65 years of age.
In conclusion, two points are important. It would aid the long-term resolution of these issues if there were a nonpartisan, broad-based public education campaign launched focusing on how Medicare works financially. Second, it would be advantageous if discussions of the financial sustainability of Medicare could be separated from public debates over reducing budget deficits or enacting tax cuts. Until these concerns are better addressed, the gaps in perception are likely to remain.
http://www.nejm.org/doi/full/10.1056/NEJMsr1307622?query=TOC
Public Often Clueless About Medicare
By David Pittman
MedPage Today, September 11, 20133
Because of a high level of misunderstanding about Medicare’s financing, lawmakers in Congress are hesitant to enact changes to the program fearing voter backlash, Bob Blendon, ScD, and John Benson, MA, both of Harvard University, wrote in a special report in Wednesday’s New England Journal of Medicine.
Ted Marmor, PhD, professor emeritus of public policy at Yale University, said it’s misleading to imply public opinion is a shaper of public policy. He called it more of a protector than a promoter.
“The public is almost never well informed about details,” Marmor told MedPage Today in a video interview. “What’s important about public opinion is what its values are and what it would be threatened by, not what it means in terms of shaping public policy in terms of direction on details.”
http://www.medpagetoday.com/PublicHealthPolicy/Medicare/41550
Public Attitudes about Medicare
Harvard School of Public Health
Poll – May 13-26, 2013
10. Which do you think is better run, (the federal Medicare program) or (private health insurance plans that people get through their jobs), or do you think they are about equally well run?
15% – The federal Medicare program
41% – Private health insurance plans
39% – About equally well run
5% – Don’t know/ Refused
19. (When you retire,) If you had a choice, would you prefer to get your Medicare health insurance benefits from the current government Medicare program, or from a private health plan, such as a PPO or HMO, offered through Medicare?
34% – From the current government Medicare program
56% – From a private health plan, such as a PPO or HMO, offered through Medicare
10% – Don’t know/ Refused
http://www.hsph.harvard.edu/horp/files/2013/06/HSPH-Medicare-Topline.pdf
Comment:
By Don McCanne, M.D. The public is not well informed on the details of Medicare. A plurality believe that private insurance plans are better run than Medicare, and a majority would prefer private plans when they retire., We should think about the political implications of this. Is “Medicare for All” really a good slogan for single payer? Medicare has some very serious defects, like it pays only about half of beneficiaries’ health expenditures. Yet we certainly don’t want a slogan that would suggest that single payer would be like private insurance for everyone. We shouldn’t change course based on the results of a single poll, but we should continue to think about how we can improve our messaging so that people do understand that single payer is what they really want. That’s true when the facts are presented, but too many still don’t understand that. As Ted Marmor implies, perhaps we should be placing more emphasis on values.
]]>New Census data on the uninsured – still 48 million
Income, Poverty, and Health Insurance Coverage in the United States: 2012
By Carmen DeNavas-Walt, Bernadette D. Proctor, Jessica C. Smith
United States Census Bureau, September 2013
Highlights
• In 2012, the percentage of people without health insurance decreased to 15.4 percent from 15.7 percent in 2011. The number of uninsured people in 2012 was not statistically different from 2011, at 48.0 million.
• Both the percentage and number of people with health insurance increased in 2012 to 84.6 percent and 263.2 million, up from 84.3 percent and 260.2 million in 2011.
• The percentage of people covered by private health insurance in 2012 was not statistically different from 2011, at 63.9 percent. This is the second consecutive year that the percentage of people covered by private health insurance was not statistically different from the previous year’s estimate. The number of people covered by private health insurance increased in 2012 to 198.8 million, up from 197.3 million in 2011.
• The percentage and number of people covered by government health insurance increased to 32.6 percent and 101.5 million in 2012 from 32.2 percent and 99.5 million in 2011.
• The percentage and number of people covered by employment-based health insurance in 2012 were not statistically different from 2011, at 54.9 percent and 170.9 million.
• The percentage and number of people covered by Medicaid in 2012 were not statistically different from 2011, at 16.4 percent and 50.9 million. The percentage and number of people covered by Medicare increased in 2012 to 15.7 percent and 48.9 million, from 15.2 percent and 46.9 million in 2011.
• Since 2009, Medicaid has covered more people than Medicare.
• In 2012, the percentage and number of uninsured children under age 18 decreased to 8.9 percent and 6.6 million, down from 9.4 percent and 7.0 million in 2011. In 2012, the uninsured rate for children in poverty, 12.9 percent, was higher than the uninsured rate for children not in poverty, 7.7 percent.
• The rate and number of uninsured non-Hispanic Whites in 2012 were not statistically different from 2011, at 11.1 percent and 21.6 million. The rate and the number of uninsured Blacks in 2012 were also not statistically different from 2011, at 19.0 percent and 7.6 million.
• The percentage of uninsured Hispanics decreased in 2012 to 29.1 percent, down from 30.1 percent in 2011. The number of uninsured Hispanics in 2012 was not statistically different from 2011, at 15.5 million.
http://www.census.gov/prod/2013pubs/p60-245.pdf
Comment:
Don McCanne, M.D.
Supporters of the Affordable Care Act (Obamacare) have been touting the improvement in our health care system since the legislation was signed into law three years ago. Well, that improvement does not apply to the numbers remaining uninsured since the minimal gains have been offset by losses, and so we still have 48 million people uninsured. That doesn’t even consider all of the injustices that remain in the maldistribution of coverage. Of course, next year’s numbers should be different. The introduction of state health insurance exchanges with government subsidies to help purchase plans and pay medical bills, plus the expansion in the Medicaid program, will reduce the numbers of uninsured. However, when Obamacare is fully implemented, the CBO estimates that 31 million people will remain uninsured. That’s a reduction of only slightly over one-third of today’s 48 million – hardly a success story for health care reform that was supposed to provide everyone with some form of insurance coverage. If we had a single payer improved-Medicare-for-all program, the number of uninsured would not be 48 million, it would not be 31 million, it would be zero! (The full Census Bureau report also includes unsettling income and poverty data. Although PNHP’s activism is limited to health care, there is so much more that needs to be done. All Americans need to make social justice our leading national priority.) Read PNHP’s press release for a brief analysis of the health insurance implications of today’s Census Bureau report: ‘Stronger medicine than Obamacare needed to end uninsured crisis’: health expert https://www.pnhp.org/news/2013/september/stronger-medicine-than-obamacare-needed-to-end-uninsured-crisis-health-expert
]]>'Stronger medicine than Obamacare needed to end uninsured crisis': health expert
Citing latest Census count of 48 million uninsured, researcher says Affordable Care Act will cut that figure by only half, leaving tens of millions vulnerable to unnecessary suffering and premature death
FOR IMMEDIATE RELEASE, Sept. 17, 2013
Contact: Mark Almberg, communications director PNHP, (312) 782-6006, mark@pnhp.org.
Local physicians in virtually every state are available for comment. (Also see 4-year historical table of state-by-state uninsured numbers, below.)
The Census Bureau’s official estimate that 48 million Americans lacked health insurance in 2012 means approximately 48,000 people died needlessly last year because they couldn’t get access to timely and appropriate care, a prominent health researcher, Dr. David Himmelstein, said today.
And contrary to many people’s expectations, the number of unprotected Americans will drop by only half when Obamacare is fully implemented – even if all the as yet undecided states were to opt-in to the law’s Medicaid expansion, he said.
The estimate of 48,000 deaths in 2012 is based on a peer-reviewed study by Himmelstein and other Harvard researchers published in the American Journal of Public Health in 2009, widely cited during the health reform debate, which found that for every 1 million persons who were uninsured there were about 1,000 related, preventable deaths.
Himmelstein is professor of public health at the City University of New York, visiting professor of medicine at Harvard Medical School, and a primary care doctor. He said, “The Census Bureau’s latest figure, 48 million uninsured, conjures up a very grim picture: a preventable death every 11 minutes.”
He said studies have shown that uninsured people with chronic illnesses like heart disease delay or forgo care, often leading to serious complications of their medical condition and, in many cases, premature death.
In another study recently published at the Health Affairs blog, Himmelstein and his colleagues found that the Affordable Care Act “will minimally alter the demographic composition of the uninsured, regardless of whether undecided states opt-in or out. While Blacks and Hispanics will continue to be overrepresented among the uninsured, the majority will be non-Hispanic, white, low-income, working-age adults, many of them employed.”
The researchers continue: “The majority … of the uninsured will be U.S. citizens, irrespective of states’ acceptance of Medicaid expansion. More than 4.3 million children and nearly 1 million veterans will remain uninsured under either scenario. … If all currently undecided states opt-in, 29.8 million people will remain uninsured [in 2016], whereas if all opt-out, the number of uninsured will total 31.0 million, 1.2 million above the opt-in scenario.”
Today’s Census Bureau report said in 2012 the percentage of people without health insurance had slightly decreased to 15.4 percent of the population from 15.7 percent in 2011, but that the number of uninsured people in 2012 was not statistically different from 2011, at 48.0 million. The bureau’s figures show the modest gains in coverage were chiefly attributable to an increase in the number of persons covered by Medicare.
While the percentage of persons covered by employment-based insurance, 54.9 percent, was not statistically different than the previous year’s figure, about a half-million fewer workers were covered by such plans in 2012.
The bureau reported that Texas had the highest percentage of uninsured, at 24.6 percent, followed by Nevada, New Mexico, and Florida, each of which exceeded 20 percent. In total numbers, California and Texas had the largest number of uninsured, each exceeding 6.4 million people.
Responding to today’s Census Bureau report, Himmelstein said: “As a physician, I simply cannot accept a situation where tens of thousands of people die every year because they lack insurance coverage. And lest anyone think this problem will be solved by Obamacare, our research and the government’s own Congressional Budget Office projections show that about 30 million people will still be uninsured in 2023. That figure translates into roughly 30,000 excess deaths annually – again, an intolerable prospect.”
Himmelstein said the nation should adopt a “zero-tolerance policy” toward lack of health coverage, and that the Census Bureau report “underscores the urgency of going beyond the Affordable Care Act and swiftly moving to a single-payer, improved-Medicare-for-all program.”
“Such a program would assure truly universal, comprehensive, high-quality coverage for everyone while simultaneously ridding us of the scourge of insurance-company-related waste, bureaucracy and profiteering,” he said. “It would thereby save both lives and money.”
Himmelstein is co-founder of Physicians for a National Health Program, an organization of 18,000 doctors who advocate for single-payer national health insurance. PNHP played no role in funding any of the research work cited above.
Four-year historical state-by-state data on the uninsured, from 2012-2009, compiled by PNHP staff from the annual findings published each fall by the Census Bureau, can be found here.
Physicians for a National Health Program (www.pnhp.org) is an educational and research organization of more than 18,000 doctors who support single-payer national health insurance. To speak with a physician/spokesperson in your area, visit www.pnhp.org/stateactions or call (312) 782-6006.
Exchange plans have sharply limited networks
Insurers limiting doctors, hospitals in health insurance market
By Chad Terhune
Los Angeles Times, September 14, 2013
The doctor can’t see you now.
To hold down premiums, major insurers in California have sharply limited the number of doctors and hospitals available to patients in the state’s new health insurance market opening Oct. 1.
New data reveal the extent of those cuts in California, a crucial test bed for the federal healthcare law.
Consumers could see long wait times, a scarcity of specialists and loss of a longtime doctor.
“These narrow networks won’t work because they cut off access for patients,” said Dr. Richard Baker, executive director of the Urban Health Institute at Charles Drew University of Medicine and Science in Los Angeles.
To see the challenges awaiting some consumers, consider Woodland Hills-based insurer Health Net Inc.
Across Southern California the company has the lowest rates, with monthly premiums as much as $100 cheaper than the closest competitor in some cases. That will make it a popular choice among some of the 1.4 million Californians expected to purchase coverage in the state exchange next year.
But Health Net also has the fewest doctors, less than half what some other companies are offering in Southern California, according to a Times analysis of insurance data.
In Los Angeles County, for instance, Health Net customers in the state exchange would be limited to 2,316 primary-care doctors and specialists. That’s less than a third of the doctors Health Net offers to workers on employer plans.
Other major insurers have pared their list of medical providers too, but not to Health Net’s degree. Statewide, Blue Shield of California says exchange customers will be restricted to about 50% of its regular physician network.
“We are nervous about these narrow networks,” said Donald Crane, chief executive of the California Assn. of Physician Groups. “It was all about price. But at what cost in terms of quality and access? Is this contrary to the purpose of the Affordable Care Act?”
Insurers and their number of doctors in L.A. County for state health exchange:
2,316 Health Net
3,009 Molina
3,855 Anthem Blue Cross
4,946 L.A. Care
5,705 Kaiser
6,559 Blue Shield PPO
8,839 Anthem EPO
28,181 Number of licensed physicians in L.A. County (MBC)
http://www.latimes.com/business/la-fi-insure-doctor-networks-20130915,0,6433104,full.story
Comment:
By Don McCanne, M.D.
These new data on use of narrow provider networks in state insurance exchanges, using Los Angeles County as an example, are important because they show us the extent to which this concept is being applied. Narrow provider networks reduce health care spending by limiting patient access to low cost providers – taking away choice – and by impairing access though supply-side contractions, that is, rationing care by limiting the supply of covered health care providers.
Another table accompanying the Los Angeles Times article (available at the link above) lists premiums for typical policies issued by these insurers for the benchmark silver plans. When comparing premiums with the numbers of physicians in the network, there are several interesting observations. Health Net, with the fewest number of physicians in their network, has the lowest premiums – no surprise. Blue Shield, California’s nonprofit Blues plan, has premiums on the lower end though it has a much larger number of physicians than does for-profit Anthem Blue Cross, yet their premiums are similar. The nonprofit seems to be more concerned about patient access whereas the for-profit seems to be concerned more about profits. However, Anthem’s EPO (exclusive provider organization) offers a larger choice in providers but extracts a much larger premium for that coverage. Comparing Anthem’s two products, it looks like if you want an accessible doctor, you’re going to have to pay for that right. Considering that Kaiser is a closed, integrated health system, it does have a fairly decent number of physicians, but it also has the highest premiums. It is likely that Kaiser’s premiums are not high because of the number of physicians, but rather they are high to prevent destabilization of their business model by allowing too many new enrollees which might strain their capacity.
Health Net’s silver plan premiums are set far enough below the others such that they will be very attractive for shoppers in the insurance exchange. The bronze plans have even lower premiums and will also be attractive. Most shoppers will be relatively healthy and will select their plans based on the premium – not on the physician networks nor on the out-of-pocket costs they would face if major health problems were to develop. Some of these people will become ill or suffer significant injuries. At that time they will discover that their choices of providers are too limited, that access may be impaired because the physicians are too busy or because they are too far away, and that the out-of-pocket expenses to which they are exposed will cause financial hardships.
Leave policy decisions to private insurers and they will always select policies that will advance their business models as opposed to policies that would provide optimal access, quality and affordability for patients. Having cheap premiums is no solution when you can’t get a doctor when you need one, and, when you finally do, you’re left broke.
Single payer would have avoided all of this, and it still can.
Taxes instead of premiums
By Ellen Oxfeld
Times Argus (Barre & Montpelier, Vt.), Letters, Sept. 16, 2013
The headline of your Sept. 5 article states, “Shumlin to rely on payroll tax hikes” to fund single payer. However, this headline would be equally accurate if it stated, “Gov. Shumlin to implement the largest single premium decrease in U.S. history.” Indeed, as the article itself makes clear, taxes to fund a health care system for all Vermonters (single payer) will replace and not add to premiums, and thus they will not constitute a hike in payments for health care at all.
Further, by replacing private premiums with public financing, we will get much more than we ever could under the current system. Let’s not forget that single payer means guaranteed health care for all Vermonters regardless of employment status. It means no more worries about going bankrupt due to high out-of-pocket costs that even the insured often face. Single payer also means greater simplicity for employers, who will no longer have to waste precious time overseeing the complex paperwork of private health care plans, as well as for providers, who will no longer have to bill many different private plans.
Our current system of patchwork coverage and fragmented financing is expensive, and despite this, we still do not have universal access to health care. Single payer means financing a health care infrastructure in a streamlined way. And it means health care will be there for all of us when we need it. That is why Gov. Shumlin is on the right track in his commitment to implementing a publicly funded health care system for all Vermonters by 2017.
Ellen Oxfeld lives in Middlebury.
http://www.timesargus.com/article/20130916/OPINION02/70916996