By Andrew Coates, M.D., F.A.C.P.
WAMC Northeast Public Radio, Dec. 6, 2013
December arrives under honking geese. As the last dying leaves find their way to the ground, frost tints the mornings, snow flurries lick the landscape, and Orion rises before bedtime. Holiday gatherings have begun. Time away from work and school might not allow us a whole day for reflection. But we might each find at least a moment of reverie or pause.
Philosophers have long explained that the world endures through a great process of dying and becoming, in the sense that everything, everyone, its at once itself and also not itself, in flux, a developing whole made up of opposites. In the words of the ancient Greek philosopher, Heraclitus: “you cannot step twice into the same stream.” Although we recognize the truth of it when we hear this ancient observation, we seldom take, or can seldom find, time to see the world in this way.
In our frenetic, pressurized social world, we cope with so many arrangements not of our making or choosing, each complete with a corporate logo and expected brand loyalty. It often seems that an expanding tangle of obligations simply fill our days. Time to step back and think about our lives runs in a trickle.
Plus, it seems strange to say “you cannot drive twice upon the same highway.” But a glimpse of ourselves as at once our old self and also the person we are becoming, changing in a changing world, even on our familiar daily commute, might be the beginning of wisdom, if we aim to develop ourselves as human beings. But when we’re a few minutes late to work, driving in traffic that is building to a clog on Albany’s 787, it seems impossible that we might think “Where are we heading?” in a metaphysical or world-historical way.
Addled by the need to change lanes, or to plan to get gasoline, or snow tires, one doesn’t take time to reflect, for example, that the Livingston Avenue railroad bridge is still in use since the post-Civil War days of Radical Republicanism, while the very highway on which we’re rolling has already require restoration from dangerous decay, since the days when Reagan was in the White House. Or that the waves just rippling an otherwise placid Hudson River announce the turning tide of the Atlantic Ocean – the very tranquil waters that told Henry Hudson’s crew that they had discovered a great estuary, not the northwest passage.
Several years back, at this time of year, I practiced medicine in Shiprock, in the Navajo Nation. We moved as a family, children and all, to New Mexico. We cherish the brief acquaintance we had with Diné culture, in which we learned to respect the breathtaking Navajo landscape as the hallowed grounds of epic human struggle. The biting winds of winter’s eve still breathe life into those experiences. It was a powerful journey, one that brought us outside of ourselves and drew us together.
While evidence of indigenous human life has been almost entirely erased from our landscape here in upstate New York, the patterns of human settlement, farming, production, and commerce established during the first centuries of colonization by Europeans etch the landscape still. Yet the past recedes so quickly. For example among our new generations very few have a connection the old ways of farm life, hand tools and homespun, in the insightful ways that earlier generations, grandchildren of immigrants and slaves, once knew.
As the cold rises from the earth and pale grays and tans emerge to soften the woods and fields before the snowfall, like the generations before us, we should take time to reflect on our species in the larger arc of history – and also the immediate social predicaments that ensnare us personally. The effort to consider what it is that might make life more worthy of the people we love prove surprisingly powerful – for each of us and for all of us.
I have glimpsed the capacity each of have to change ourselves. Among the many indelible experiences brought to my life by the privilege of being a physician, attending the death of patients has taught me about people. In the face of the death of a family member, friend or even a stranger, people rise to the occasion. With death an irrevocable change occurs – and human beings reach inside, summon appropriate emotion, muster personal courage, as well as community resources of human solidarity – and then they transcend.
A time is coming when we will find that we simply must move forward to transcend our present social and environmental predicaments – personally and also as species. For today, a moment of personal reflection can help us meet that coming challenge.
Dr. Andrew Coates practices internal medicine in Upstate New York. He is president of Physicians for a National Health Program.
You can listen to Dr. Coates’ radio broadcast here: http://wamc.org/post/andrew-coates-time-reflect
Medicare system for all best health care option
By Marc Lavietes, M.D.
Asbury Park (N.J.) Press, Dec. 5, 2013
Frustration with the rollout of The Affordable Care Act is understandable. We should remember that similar problems and criticisms were rampant when the Medicare program was initiated.
In fact, conflict over the proper role of government in health care reflects the classic American debate regarding the role of government per se. This Jeffersonian-Hamiltonian debate is named after the most prominent proponents of either side. Despite the dire warnings, Medicare has been successful.
Most important, readers should note these basic truths. Fifty million Americans have no health insurance. Fifty million more have grossly inadequate insurance. Only the wealthiest of Americans can survive the economic hardship accompanying a profound illness. Even in Massachusetts with an “Obamacare-like” health care system already in place, severe illness remains the major cause of personal bankruptcy.
Maintaining our current health care delivery system, as suggested by some letter writers, best serves only those few Americans who profit from it. All other industrial countries provide better health care to their citizens at substantially lower costs. This truth is often dismissed by our mainstream media under the pretext of “socialized medicine.”
While the outcome of the current battles over health care is unclear, it seems likely that those more progressive states having formed their own marketplaces will provide improved care to their citizens, albeit without cost savings. By contrast, the quality of health care in the remaining states will deteriorate. In the final analysis an improved “Medicare for all” system is the best answer.
Dr. Marc H. Lavietes resides in Bradley Beach, N.J.
http://www.app.com/article/20131205/NJOPINION02/312050027/Medicare-system-for-all-best-health-care-option?nclick_check=1
10 Questions: Steven Nissen, M.D.
By Todd Neal, Senior Staff Writer
MedPage Today, Dec. 5, 2013
What’s the biggest barrier to practicing medicine today? That’s just the first of 10 questions the MedPage Today staff is asking leading clinicians and researchers to get their personal views on their chosen profession. In this series we share their uncensored responses. Here, answers from Steven Nissen, MD, of the Cleveland Clinic.
There, Nissen is chair of the Robert and Suzanne Tomsich Department of Cardiovascular Medicine. A past president of the American College of Cardiology and former chair of the FDA’s Cardiovascular Renal Drugs Advisory Committee, he has had a leading role in highlighting potential risks associated with certain drugs, including rofecoxib (Vioxx) and rosiglitazone (Avandia). In 2007, Nissen was included on Time Magazine‘s list of “100 men and women whose power, talent, or moral example is transforming the world.”
1. What’s the biggest barrier to your practicing medicine today?
The lack of a single-payer system. We waste enormous amounts of time and energy dealing with insurance companies, whose major goal is figuring out how not to cover patients.
2. What is your most vivid memory involving a patient who could not afford to pay for healthcare (or meds or tests, etc.) and how did you respond?
There are too many to count. I remember a patient who could not afford clopidogrel (Plavix), so he split his pills to stretch the prescription, but subsequently had a catastrophic in-stent thrombosis leading to cardiogenic shock and eventually heart transplantation.
3. What do you most often wish you could say to patients, but don’t?
If you continue to smoke, I would prefer that you see another physician.
4. If you could change or eliminate something about the healthcare system, what would it be?
Fee-for-service medicine. It drives overutilization and leads to poor outcomes.
5. What is the most important piece of advice for med students or doctors just starting out today?
Consider a career in academic medicine. It provides greater diversity and satisfaction than limiting your career to clinical practice.
6. What is your “elevator” pitch to persuade someone to pursue a career in medicine?
I have never regretted my decision. The relationship to patients as well as science makes medicine a unique career choice.
7. What is the most rewarding aspect of being a doctor?
The appreciation we receive from patients and their families. It’s always very special.
8. What is the most memorable research published since you became a physician and why?
I actually think the CAST Trial was most memorable. It continues to resonate. Drugs that suppressed arrhythmias increased the rate of death. It began the ongoing movement away from surrogate endpoints.
9. Do you have a favorite hospital-based TV show?
I don’t watch TV (except the NewsHour on PBS). Television lowers your IQ substantially. There’s a dose-response curve. The more you watch, the more stupid you become.
10. What is your advice to other physicians on how to avoid burnout?
If you can, do what you really enjoy. Then work becomes a pleasure.
Todd Neal is senior staff writer at MedPage Today. http://www.medpagetoday.com/PracticeManagement/PracticeManagement/43257?isalert=1&uun=g441580d398R5538349u&utm_source=breaking-news&utm_medium=email&utm_campaign=breaking-news&xid=NL_breakingnews_2013-12-05
]]>Wall Street’s view of narrow networks
HSC’s 18th Annual Wall Street Comes to Washington Conference
Center for Studying Health System Change, November 21, 2013 From the conference transcript: Paul Ginsburg (President, Center for Studying Health System Change): Let me move on to network innovations. And one thing that came up a little bit in our first session was narrow- or limited-network products. And let me start by asking about how are plans building limited networks? I mean, in a sense, what are they looking for as far as which providers would they like to have? How sophisticated are they in assessing the value of different providers? Carl McDonald (Director and Senior Analyst, Citi Investment Services): I can go quick: Price. I’m done. Paul Ginsburg: Okay. Actually, how sophisticated is the price? Carl McDonald: Sorry? “How sophisticated…” Paul Ginsburg: How sophisticated is the price? Is it price per episode? Is it simply, you know, unit prices? Carl McDonald: Yes, I mean, generally it’s going to be the unit price, or price per episode. Matthew Borsch (Vice President, Goldman Sachs): Let me just offer one thing that’s happening. This is not quite to the tiered-network strategy, or narrow-network strategy, per se, but it’s topical right now in that you’ve seen some of the health plans in Medicare Advantage taking some pretty strong steps to narrow their networks. On the physician side, it’s been the most notable. In fact, there was a, there’s been some communication about that. There was a letter that was posted yesterday from the health insurance industry to CMS, stressing how important it was for the plans to be able to make these network exclusions. But obviously, for doctors who’ve been, you know, contracted in Medicare Advantage to suddenly be, to be terminated, where, in most cases, they continue to participate on the commercial side, has created some real blowback. Paul Ginsburg: I had noticed that, and was wondering, it sounded to me that this was different way that a plan pursues a more limited network. Matthew Borsch: It is. Paul Ginsburg: It seems as though, and I saw The Wall Street Journal article a week or two ago about United, and it almost seemed as though they were trying to get their star quality scores up by culling out the physicians who contribute to low scores. And is that what it’s about, Matt? Matthew Borsch: Well, the truth is we don’t really know. Paul Ginsburg: Yeah. Matthew Borsch: You know, that, that is, from our perspective, somewhat of a black box, in terms of the decision making there. There are multiple criteria. There’s how each physician group feeds into the star quality scores. There are utilization, efficiency metrics that they can run on a broad, you know, larger companies can run on a broad set of claims data. There’s also, frankly, the consideration of which Medicare Advantage members are assigned to those physician groups. And again, I’m not pointing to any one of these three as a factor but there you could possibly have some effort to change the risk distribution of the underlying membership. Sheryl Skolnick (Managing Director & Co-Head of Research, CRT Capital Group): So, just to put this in context, Medicare Advantage rates are coming down very significantly next year. They’re actually going down next year from United’s perspective, what? about 3 1/2 percent or so. And when your rates go down, some of your plans, and some of your providers in those plans will have to be terminated, because you need to essentially shrink to a profitable size, or a sustainable size. So that’s part of what you’re seeing, is instead of the proactive “We’re introducing a new benefit plan, we’re going to build a narrow network,” now you’re seeing the reactive effect of United’s always been a very inclusive and broad based network. They’ve had some issues of adverse publicity in St. Louis and some other places when they’ve tried to narrow the network based on quality. There is a lot less push back on that sort of thing now. But they’re getting some push back on this one because in Connecticut alone, for example, it’s 2,000 providers. That’s a lot in Connecticut. It’s not that big a state. So, what you’re seeing is, first, the unwinding. Second, I agree with you completely, I think it is absolutely a strategy to get their star scores up, because they’re a major embarrassment. And they’re clearly, from their last conference calls, a focus of the company strategy for Medicare Advantage for the next couple of years, is to get the star scores up. But I also, I agree with Matt, that there are many other factors at work, most notably that they need to get all of these markets that they’ve expanded rather broadly to get rid of the marginal plan, to get rid of the marginal provider and, in some cases, the high cost member. Robert Berenson (Institute Fellow, The Urban Institute): But I think it’s important to point to a major difference between the Medicare managed care situation and commercial, which is that in Medicare, out of network services are paid at Medicare rates, so that changes the whole leverage situation. And it’s the reason, I think, that hospitals basically are in network at Medicare rates, or near to Medicare rates, because they don’t have the leverage. Balance billing is a whole different situation. I’m actually surprised that MA plans weren’t more aggressive in the past, because they have the protection for the out of network care. And others, there won’t be such push back from the beneficiaries hit with the complete balance bill, if their physician is not in network, or something like that. Paul Ginsburg: So, getting into the employer based, the commercial space, you know, it looks like there’s been substantial growth in small group plans to have narrow networks. And, of course, so many of the products of the exchanges are narrow networks. And, any comments about that strategy, how it’s going, is there going to be, is there going to be push back by the public? Sheryl Skolnick: For a long time the hospitals were telling us that while Wall Street was busy talking about the narrowing of networks, they weren’t actually seeing it. It was only when the exchange contracts came up that, even in the beginning, there was some concern that some of the contracts that were being signed weren’t narrow-network contracts, in the very beginning of the contracting. Towards the end of the contracting for reform these are commercial, by the way, these are fundamentally commercial contracts. So, by the end of the contracting, though, almost all of the contracts being signed were for some sort of a narrowed network. So, I think there was a very quick evolution in the thought process of the plans in negotiating these things, where they very quickly realized: This is one of the very few levers we have, we better pull it. Paul Ginsburg: Yes. And, to what extent, as they form these networks, to what extent are the savings going to come from keeping high cost providers out, or getting discounts from providers? Sheryl Skolnick: Yes. Yes. Paul Ginsburg: Which is the dominant piece, or are they both very important. Sheryl Skolnick: Very important. Paul Ginsburg: Okay. That’s the answer. http://www.hschange.org/CONTENT/1396/?id_conf=32
Comment:
By Don McCanne, M.D. If insurers were marketing products designed primarily to get their clients the health care that they need, you would think that they would do their best to make sure that they cover essentially all of the physicians that their clients would select. But they don’t, and they are narrowing even further their lists of contracted providers. Why? Wall Street understands. It ’s not about quality or access. It’s about the money.
]]>More health care regulations mean more middlemen, fewer doctors
By Stephen B. Kemble, M.D.
Honolulu Star-Advertiser, Nov. 27, 2013
I attended the recent Hawaii 2013 Healthcare Summit, on how Hawaii is implementing the Affordable Care Act and transforming health care. The keynote address by Dr. Abraham Verghese was inspiring — all about the sanctity of the doctor-patient relationship and how health care should be focused on the living patient, not the “iPatient” in the computer.
In panel discussions, Hawaii’s health plans and hospitals told us how they will guide us away from fee-for-service payment that rewards volume of services to value-based payment systems that reward quality and care coordination. The goals are the “triple aims” of improved quality, improved population health, and improved value/reduced cost. However, dig deeper and the conference was full of contradictions and confusion.
Information presented included:
* Hawaii has a low rate of medical procedures compared to the rest of the country.
* We have the lowest per capita fee-for-service Medicare expenditures in the country.
* Thanks to relatively broad coverage under our Prepaid Health Care Act, Hawaii covers more of our population than any state besides Massachusetts — our benefits are already at the “gold” and “platinum” levels for Obamacare plans, better than any other state — yet we have the third lowest insurance premiums in the country, and all of this under a fee-for-service system.
* Hawaii has 20 percent fewer physicians than needed for our population and this is projected to get worse. Shortages are especially severe on the neighbor islands.
* Two-thirds of Hawaii psychiatrists no longer accept new Medicaid patients, many dropping out in the past four years, and our ER and hospital costs for mental illness have risen 30 percent in that time.
Hospitals and health plans were well represented on panels, but no practicing doctors. Doctors were shaking their heads as panelists told us that solo and small-group medical practices will soon become extinct, replaced by competing “accountable care organizations.” Every health plan and hospital now has multiple “partners” deploying computerized systems to enable them to better manage health care. Doctors are going to be rewarded for meeting quality metrics and punished with financial penalties if they fail to purchase computer systems that achieve “meaningful use,” or if they fail to meet quality metrics.
You would think from these presentations that the problem is doctors who don’t care about quality and just want to do more procedures and see more patients to make more money. The health insurance plans and hospitals are going to make sure doctors get paid for “quality,” not “volume.” However, there is no evidence for the alleged problem with excessive “volume” of services here, and if you look at the actual “quality” metrics, they are either very narrow, focusing on those limited aspects of health care that can be easily measured, or they are seriously flawed and don’t actually measure “quality.”
The managers and middlemen in health care are proliferating while our supply of doctors is dwindling. The evidence shows that doctors in Hawaii are not actually delivering much unnecessary care, but there are not enough of them and the ones we have are overworked and overburdened with administrative requirements. We are apparently pursuing Dr. Verghese’s “iPatients” at the expense of real patients.
Doctors agree that time spent on charting and administration is increasing, so they must work longer hours, spend less time with each patient, or see fewer patients. They are restricting their practices to fewer insurance plans to control administrative burdens, leaving more patients with inadequate access to care. Many are talking about early retirement or dropping participation with health insurance entirely, converting to “concierge” practices for those who can afford it. All of this is taking us in the opposite direction from the “triple aim” goals.
Most of our problems are problems with inadequate access to care, especially for those with Medicaid, not fee-for-service incentives or lack of concern for quality.
Hawaii’s experience with our Prepaid Health Care Act shows that broader coverage and improved access to care actually reduce health care costs. Let’s take this further and expand coverage to everyone, build our health care provider work force, simplify and streamline administration, pay doctors the same for everyone, and eliminate barriers to access care. Single payer, anyone?
Stephen B. Kemble, M.D., is a psychiatrist, an assistant professor at the John A. Burns School of Medicine and immediate past president of the Hawaii Medical Association.
http://www.staradvertiser.com/s?action=login&f=y&id=233570491
Pritzker students explore single-payer health care at PNHP national conference
By Pamela Peters, MS1
Pritzker News, University of Chicago Pritzker School of Medicine, December 4, 2013
With the recent enactment of key portions of the Affordable Care Act, health care reform has increasingly become a hot-button issue. Six students from Pritzker explored the option of single-payer health care reform by attending the annual meeting for the advocacy group Physicians for a National Program (PNHP) on November 2, 2013 in Boston. PNHP is a non-p rofit research and education organization of 19,000 physicians, medical students, and health professionals based in Chicago with chapters in almost every state. The turnout at the meeting set a new record for the organization, with 404 registrants from 38 states.
“The conference was a great opportunity to discuss the economic and medical realities of health care going forward under the ACA, as well as the role of physicians in pushing for change in how medical care is financed,” commented Brandon Berger, MS1. “To me, single payer is a solution to the prohibitive cost of health care, an opportunity to provide medical care in a way that doesn’t discriminate based on ability to pay, and a public health initiative of enormous potential impact.”
At the meeting, Pritzker students had the opportunity to listen to presentations from a variety of speakers, such as Vermont Governor Peter Shumlin, who outlined progress and barriers in creating a single-payer health care system for his state. Dr. Marcia Angell, former editor of the New England Journal of Medicine, gave a talk entitled, “Patients and Profits,” and PNHP co-founders Dr. David Himmelstein and Dr. Steffie Woolhander updated attendees with the most recent statistics about the status of health care in America.
rofit research and education organization of 19,000 physicians, medical students, and health professionals based in Chicago with chapters in almost every state. The turnout at the meeting set a new record for the organization, with 404 registrants from 38 states.
“The conference was a great opportunity to discuss the economic and medical realities of health care going forward under the ACA, as well as the role of physicians in pushing for change in how medical care is financed,” commented Brandon Berger, MS1. “To me, single payer is a solution to the prohibitive cost of health care, an opportunity to provide medical care in a way that doesn’t discriminate based on ability to pay, and a public health initiative of enormous potential impact.”
At the meeting, Pritzker students had the opportunity to listen to presentations from a variety of speakers, such as Vermont Governor Peter Shumlin, who outlined progress and barriers in creating a single-payer health care system for his state. Dr. Marcia Angell, former editor of the New England Journal of Medicine, gave a talk entitled, “Patients and Profits,” and PNHP co-founders Dr. David Himmelstein and Dr. Steffie Woolhander updated attendees with the most recent statistics about the status of health care in America.  Pritzker students also had the opportunity to attend many student-specific workshop sessions, where medical students from around the country shared inspiring stories of activism and counseled newcomers on how to become more involved in the single-payer movement. Pritzker’s very own Scott Goldberg, MS2, who is a student delegate on the PNHP national board of directors, led a session entitled “Heroism vs. Evil in Medicine: Transitioning from Sympathizer to Activist.” Scott also founded the University of Chicago student chapter of PNHP, and spent time working with PNHP California this past summer to advocate for movement towards a state-based, single-payer health care system there.
“I have seen the medical student movement for single-payer grow significantly in just one year since the last PNHP annual meeting, commented Scott. “The 140 students in attendance were organized, inspired, and committed to fighting for truly universal health insurance. The Affordable Care Act has a few strengths, but it does not fundamentally reform our costly, inefficient, unjust health care system. It still treats health care as a commodity to be traded not a public good. While single-payer reform may seem inevitable to some, it will only occur through the tireless efforts of medical students, physicians, and health professionals. I was honored to lead a workshop that could offer students some tools and insights into making that leap from advocate to activist.”
The conference included an additional day of Leadership Training for those who were new to single payer or wanted to learn how to better discuss it with others. The Leadership Training was held on November 1 and began with instruction on how to present the concept of single payer health care in a Grand Rounds format. Three Pritzker students (Brandon Berger, MS1; Rachel Stones, MS1; Pamela Peters, MS1) were able to attend this workshop through generous scholarships from either the Nicholas Skala Student Activist Scholarship fund or the Illinois Single Payer Coalition.
Pritzker students also had the opportunity to attend many student-specific workshop sessions, where medical students from around the country shared inspiring stories of activism and counseled newcomers on how to become more involved in the single-payer movement. Pritzker’s very own Scott Goldberg, MS2, who is a student delegate on the PNHP national board of directors, led a session entitled “Heroism vs. Evil in Medicine: Transitioning from Sympathizer to Activist.” Scott also founded the University of Chicago student chapter of PNHP, and spent time working with PNHP California this past summer to advocate for movement towards a state-based, single-payer health care system there.
“I have seen the medical student movement for single-payer grow significantly in just one year since the last PNHP annual meeting, commented Scott. “The 140 students in attendance were organized, inspired, and committed to fighting for truly universal health insurance. The Affordable Care Act has a few strengths, but it does not fundamentally reform our costly, inefficient, unjust health care system. It still treats health care as a commodity to be traded not a public good. While single-payer reform may seem inevitable to some, it will only occur through the tireless efforts of medical students, physicians, and health professionals. I was honored to lead a workshop that could offer students some tools and insights into making that leap from advocate to activist.”
The conference included an additional day of Leadership Training for those who were new to single payer or wanted to learn how to better discuss it with others. The Leadership Training was held on November 1 and began with instruction on how to present the concept of single payer health care in a Grand Rounds format. Three Pritzker students (Brandon Berger, MS1; Rachel Stones, MS1; Pamela Peters, MS1) were able to attend this workshop through generous scholarships from either the Nicholas Skala Student Activist Scholarship fund or the Illinois Single Payer Coalition.

“It was refreshing to be around so many doctors and students who are passionate and actively working towards a more equitable health care system,” said Rachel. “I became much more informed about single-payer and I will definitely be continuing the learning process. I was also inspired by the things that medical students are doing and the activism they are involved with around the country.”
Whether new to activism or a health policy and advocacy veteran, all who attended the conference benefited greatly from the thought-provoking presentations and the equally stimulating dialogues that followed them. http://pritzker.uchicago.edu/about/news/PNHP-Conf.shtml
]]>Nobody Should Get Rich Off Obamacare
By Evan Soltas
Bloomberg, The Ticker, Dec. 3, 2013
For an industry that’s supposed to be burdened by the launch of Obamacare, the health-care business is doing pretty well. Stocks of health-care companies are up almost 40 percent this year, the strongest performance of any sector in the S&P 500.
This is despite, for insurers, new regulations on the “medical loss ratio” which require them to spend at least 80 percent of premiums on health care — in practice, capping their profits and administrative expenses such as advertising at 20 percent. How about the medical-technology manufacturers that were slapped with an excise tax? Doing just fine. The hospital chains that face lower reimbursement rates from Medicare patients? They’re doing well, too.
Health care is a business, and businesses are supposed to make money. Still, it’s a bit concerning that health-care investors are so upbeat just as President Barack Obama’s health-reform law goes into effect.
It makes you wonder where the new profits are expected to come from. If they’re earned in a competitive market, great — but health care in the U.S. hasn’t been a free market in decades, so it’s worth turning a skeptical eye.
The law will give the insurance industry millions of new customers and subsidizes its products. It brings millions of others into the market for health-care services through its Medicaid expansion. If health-care investors are throwing a party, it might be because the rest of us are paying for it.
Economists call profits in excess of what would be earned in a competitive market “rents.” Often it’s hard to tell the difference — but the expected increase in health-care profits has a whiff of rent about it. After all, Obama passed his law with the support of the health-care industry. The insurers signed on. Pharma signed on. Doctors signed on. It would be shocking if this law reduced their rents.
Regulation is the usual remedy. Public utilities commissions, for example, determine the “fair profit” of electric utilities and prevent them from squeezing customers. In health care, this hasn’t been the Obama administration’s approach. A headline on a recent piece by Adam Davidson put it best: “The President Wants You To Get Rich On Obamacare.” It said that Tom Scully, a private-equity executive who has been pitching health-care investments, leaves investors expecting a gold mine:
No matter what investors thought about Obamacare politically — and surely many there did not think much of it — the law was going to make some people very rich. … With the right understanding of the industry, private-sector markets and bureaucratic rules, savvy investors could help underwrite innovative companies specifically designed to profit from the law. Billions could flow from Washington to Wall Street, indeed.
The health-care reform gives health-care suppliers one of the benefits enjoyed by utilities: safe profits. But the quid pro quo — that those profits should be moderate — seems to be missing. That’s the assessment of investors, anyway. For now, at least, they aren’t looking at Aetna the way they look at Con Ed.
Evan Soltas is a contributor to the Ticker.
http://www.bloomberg.com/news/2013-12-03/nobody-should-get-rich-off-obamacare.html?alcmpid=view
]]>Who wins under Obamacare?
Nobody Should Get Rich Off Obamacare
By Evan Soltas
Bloomberg View, December 3, 2013
For an industry that’s supposed to be burdened by the launch of Obamacare, the health-care business is doing pretty well. Stocks of health-care companies are up almost 40 percent this year, the strongest performance of any sector in the S&P 500.
How about the medical-technology manufacturers that were slapped with an excise tax? Doing just fine. The hospital chains that face lower reimbursement rates from Medicare patients? They’re doing well, too.
Health care is a business, and businesses are supposed to make money. Still, it’s a bit concerning that health-care investors are so upbeat just as President Barack Obama’s health-reform law goes into effect.
The law will give the insurance industry millions of new customers and subsidizes its products. It brings millions of others into the market for health-care services through its Medicaid expansion. If health-care investors are throwing a party, it might be because the rest of us are paying for it.
http://www.bloomberg.com/news/2013-12-03/nobody-should-get-rich-off-obamacare.html?alcmpid=view
Comment:
By Don McCanne, M.D. To pass the Affordable Care Act, President Obama was convinced that he had to gain the support of the health financing and health care industries. He did. Look who’s profiting. Who loses? Those who will have to pay much more out of pocket for health care because of higher deductibles. Those who lose choice of their physicians and hospitals because of narrower provider networks, and end up losing catastrophic protection because of care inadvertently received out of network. Those who will be contributing through taxes or insurance premiums far more than they should have to because of the profoundly wasteful administrative excesses of our dysfunctional financing system. That’s most of us. The improvements in insurance plans for the few – guaranteed issue and community rating – do not begin to offset the deterioration that is beginning to take place in the employer-sponsored plans where most of us receive our health care coverage. There are a few of us who will gain, some by being enrolled in Medicaid and some by receiving subsidies for exchange plans, but the numbers of us who will lose is far greater than the numbers who will win. We could have had reform in which we would all be winners – an improved Medicare that covers everyone. Even those who will gain through Medicaid or subsidies would gain much more under a single payer system. But no, political feasibility dictated that the vested stakeholders of the medical-industrial complex be the ones who get the money, while the rest of us pay more and get less.
]]>Medicare for all is the solution
By Andrew Rock
Tampa Bay Times, Letters, Nov. 3, 2013
Re “New dispute arises: policy cancellations” (Oct. 30)
All the recent hoopla about the Affordable Care Act has generated a lot of heat but not much light. In all the angry finger-pointing, both parties have missed the main point. Obamacare is flawed and cumbersome for the same reason that our existing “system” doesn’t work: It is a health insurance system, not a health care system. The obvious answer is a single-payer health care system, Medicare for all
The administration is running into problems with technology and with cancellation of existing policies precisely because Obamacare is an insurance-based program. So we have to navigate insurance exchange websites, that must then connect up with insurance company databases, that must then correlate with existing insurance coverage, and so on. It’s bound to be inefficient and confusing, and also costly.
Insurance companies take at least 20 cents out of every dollar Americans spend on health care; Medicare takes only 2 or 3 cents on the dollar. Health insurance companies are massively profitable, yet most Americans either can’t afford health insurance or are very dissatisfied with the coverage they have, which is not only expensive but often not there for us when we need it most.
Those Americans fortunate enough to be on Medicare are very happy with it. Most of us, including President Barack Obama, knew that a single-payer Medicare for all system was by far the best way to reform American health care. But it didn’t happen because it wasn’t “politically doable.” Most of our congressmen and state legislators are more responsive to the corporate interests who pay for their election campaigns than the people they claim to represent. This is true of both Republicans and Democrats. So single payer was never on the table because the health insurance lobby is simply too powerful.
If Obamacare ever gets off the ground, it will be helpful to many low-income Americans who will be able to afford health insurance. But it is a huge windfall for the health insurance industry, just as the Bush administration’s prescription drug benefit was a huge windfall for the pharmaceutical industry.
Andrew Rock lives in Tampa.
http://www.tampabay.com/opinion/letters/vote-for-november-letter-of-the-month/2155085
]]>Bone Marrow as a commodity
Why It’s OK to Pay Bone-Marrow Donors
By Sally Satel
Bloomberg View, December 1, 2013
Locating a marrow donor is often a needle-in-a-haystack affair. The odds that two random individuals will have the same tissue type are less than 1 in 10,000, and the chances are much lower for blacks.
Allowing compensation for donations could enlarge the pool of potential donors and increase the likelihood that compatible donors will follow through. So the ruling by a three-judge panel of the U.S. Court of Appeals for the Ninth Circuit was promising news for the 12,000 people with cancer and blood diseases currently looking for a marrow donor.
Shaka Mitchell, a lawyer in Nashville, Tennessee, and co-founder of the nonprofit MoreMarrowDonors.org… invited a team of economists to evaluate the effects of the ruling on people’s willingness to join a registry and to donate when they are found to be a match. The researchers were to specifically assess whether cash payments would be any more or less persuasive than noncash rewards or charitable donations.
Now comes the bad news. On Oct. 2, the U.S. Department of Health and Human Services proposed a new rule that would overturn the Ninth Circuit’s decision. The government proposes designating a specific form of bone marrow — circulating bone-marrow stem cells derived from blood — as a kind of donation that, under the 1984 National Organ Transplant Act, cannot be compensated.
The strongest opposition to compensation comes from the National Marrow Donor Program, the Minneapolis-based nonprofit that maintains the nation’s largest donor registry. Michael Boo, the program’s chief strategy officer, says of reimbursement, “Is that what we want people to be motivated by?”
HHS is presumably under pressure from the National Marrow Donor Program. The department does not otherwise explain its proposed rule except to claim that compensation runs afoul of the transplant act’s “intent to ban commodification of human stem cells” and to “curb opportunities for coercion and exploitation, encourage altruistic donation and decrease the likelihood of disease transmission.”
Each year, 2,000 to 3,000 Americans in need of marrow transplants die waiting for a match. Altruism is a virtue, but clearly it is not a dependable motive for marrow donation.
(Sally Satel, is a psychiatrist and a resident scholar at the American Enterprise Institute.)
http://www.bloomberg.com/news/2013-12-01/why-it-s-ok-to-pay-bone-marrow-donors.html
Comment:
By Don McCanne, M.D. Imagine trading bone marrow in the commodities market. It could be very lucrative. In no time at all, the prices could be driven over what we are now paying for the newer cancer drugs – $100,000 and more – maybe much more. And don’t stop at bone marrow. Think of the trade that could be generated in other human organs. Is there no end to the commodification of health care? How did we end up here? Is the compulsion to look for market solutions so great that we abandon all sense of humanity? People who think like this – do they have a soul?
]]>The real fix for Obamacare's flaws: Medicare for all
There’s no reason to rollback the progress the ACA has made. But we should go all the way and dump the for-profit system
By RoseAnn DeMoro
The Guardian (U.K.), Nov. 27, 2013
Lost amidst the well-chronicled travails of the Affordable Care Act rollout are the long term effects of people struggling to get the health coverage they need without going bankrupt.
If that sounds familiar, it’s because that’s been the main story line of the US healthcare system for several decades. Sadly, little has changed.
Still, with all the ACA’s highly publicized snafus, and less discussed systemic flaws, there’s no reason to welcome the cynical efforts to repeal or defund the law by politicians whose only alternative is more of the same callous, existing market-based healthcare system.
US nurses oppose the rollback and appreciate that several million Americans who are now uninsured may finally get coverage, principally through the expansion of Medicaid, or access to private insurance they’ve been denied because of their prior health status.
At the same time, nurses will never stop campaigning for a fundamental transformation to a more humane single-payer, expanded Medicare for all system not based on ability to pay and obeisance to the policy confines of insurance claims adjustors.
Website delays – the most unwelcome news for computer acolytes since the tech boom crashed – are not the biggest problem with the ACA, as will become increasingly apparent long after the signup headaches are a distant memory.
What prompted the ACA was a rapidly escalating healthcare nightmare, seen in 50 million uninsured, medical bills plunging millions into un-payable debt or bankruptcy, long delays in access to care, and record numbers skipping needed treatment due to cost.
The main culprit was our profit-focused system, with rising profiteering by a massive health care industry, and an increasing number of employers dropping coverage or just dumping more costs onto workers.
The ACA tackles some of the most egregious inequities: lack of access for many of the working poor who will now be eligible for Medicaid or subsidies to offset some of their costs for buying private insurance through the exchanges, a crackdown on several especially notorious insurance abuses, and encouragement of preventive care.
But the law actually further entrenches the insurance-based system through the requirement that uncovered individuals buy private insurance. It’s also chock full of loopholes.
Some consumers who have made it through the website labyrinth have found confusing choices among plans which vary widely in both premium and out of pocket costs even with the subsidies, a pass through of public funds to the private insurers.
The minimum benefits are also somewhat illusory. Insurance companies have decades of experience at gaming the system and warehouses full of experts to design ways to limit coverage options.
The ACA allows insurers to cherry pick healthier enrollees by the way benefit packages are designed, and as a Washington Post article noted on 21 November, consumers are discovering insurers are restricting their choice of doctors and excluding many top ranked hospitals from their approved “network”.
The wide disparity between the healthcare you need, what your policy will cover, and what the insurer will actually pay for remains.
Far less reported is what registered nurses increasingly see – financial incentives within the ACA for hospitals to prematurely push patients out of hospitals to cheaper, less regulated settings or back to their homes. It also encourages shifting more care delivery from nurses and doctors to robots and other technology that undermines individual patient care, and that may work no better than the dysfunctional ACA websites.
Is there an alternative? Most other developed nations have discovered it, a single-payer or national healthcare system.
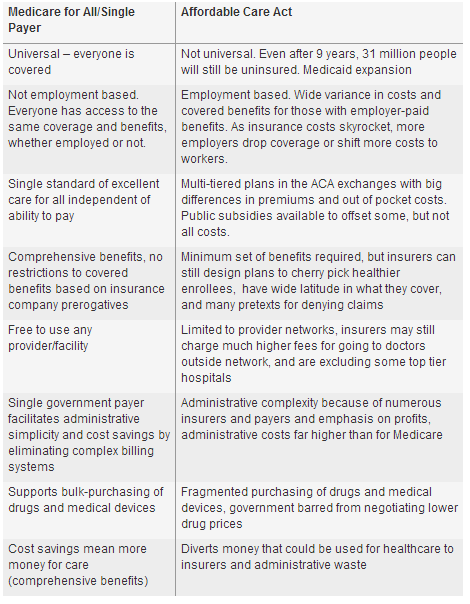
Without the imperative of prioritizing profits over care, Medicare for all streamlines the administrative waste and complex insurance billing operations endemic to private insurance. That waste is a major reason why the US has more than double the per capita cost of healthcare of other developed nations, yet lower life expectancies than many.
Medicare for all eliminates the multi-tiered health plans that plague both the individual and group insurance markets that are tied to the girth of your wallet not your need for care. Class, gender, and racial disparities in access and quality of care vanish under Medicare for all.
It’s beyond time that we stop vilifying government and perpetuating a corporatized healthcare system that has abandoned so many. We can, with a system of Medicare for all, we can cut healthcare costs and promote a much more humane society.
http://www.theguardian.com/commentisfree/2013/nov/27/obamacare-flaws-medicare-for-all
]]>Grading a Physician's Value — The Misapplication of Performance Measurement
Grading a Physician’s Value — The Misapplication of Performance Measurement
By Robert A. Berenson, M.D., and Deborah R. Kaye, M.D.
The New England Journal of Medicine, November 28, 2013
Perhaps the only health policy issue on which Republicans and Democrats agree is the need to move from volume-based to value-based payment for health care providers. Rather than paying for activity, the aspirational goal is to pay for outcomes that take into account quality and costs. In keeping with this notion of paying for value rather than volume, the Affordable Care Act (ACA) created the “value-based payment modifier,” or “value modifier,” a pay-for-performance approach for physicians who actively participate in Medicare. By 2017, physicians will be rewarded or penalized on the basis of the relative calculated value of the care they provide to Medicare beneficiaries.
Although we agree that value-based payment is appropriate as a concept, the practical reality is that the Centers for Medicare and Medicaid Services (CMS), despite heroic efforts, cannot accurately measure any physician’s overall value, now or in the foreseeable future.
The value modifier is meant to provide differential payment to a physician or physician group under the Medicare Physician Fee Schedule on the basis of the quality of care furnished as compared with the cost. To reduce the burden on physicians, CMS has based the value modifier on the Physician Quality Reporting System (PQRS).
The meager rate of physician participation in the PQRS suggests that something is fundamentally wrong — physicians simply do not respect the measures, and for good reason. PQRS measures reflect a vanishingly small part of professional activities in most clinical specialties. A handful of such measures can provide a highly misleading snapshot of any physician’s quality. Research shows that performance on specific aspects of care does not predict performance on other components of care. Primary care physicians manage 400 different conditions in a year, and 70 conditions account for 80% of their patient load. Yet a primary care physician currently reports on as few as three PQRS measures.
The challenge of accurately assigning costs to an individual physician is similarly daunting. Current methods for case-mix adjustment do not adequately capture variations in patients’ illness severity, complicating coexisting conditions, or relevant socioeconomic differences — differences beyond the physician’s control that affect the cost of care. And we currently don’t know how to attribute to an individual physician the costs that Medicare beneficiaries generate across the health care system.
Even if we had better measures, behavioral economists would still challenge the pay-for-performance concept, at least for professionals such as physicians and teachers, who must manage complex situations and creatively solve problems. These critics argue that rewarding professionals on the basis of a particular performance measure has the potential to crowd out the intrinsic motivation to perform well across the board, not just on the few activities being measured.
http://www.nejm.org/doi/full/10.1056/NEJMp1312287?query=TOC
Comment:
By Don McCanne, M.D. The “value-based payment modifier” – an adjustment in payments to reward physicians for improving value in the health care they provide, or to punish them for providing lower value – is yet another example of the often misguided measures in the Affordable Care Act allegedly designed to improve our health care system, when, in fact, the fundamental reforms in the health care financing system that we really needed were barely touched upon, in deference to the private insurance industry. It will be difficult to change from a volume-based system (fees based on volume of services provided) to a value-based payment system when we still do not know how to define the value of physician services, as Drs. Berenson and Kaye explain to us in this NEJM article, though they do suggest some other modest measures that might have some benefit. It is fine to continue research on measures that have a potential for improving value in health care, but it is almost criminal to ignore a concept that has already been proven in other nations to dramatically increase value – potentially a far greater increase than all of the other measures combined that are included in the Affordable Care Act. Of course, that concept is single payer financing. Let’s first enact an improved Medicare for all, and then we could tweak the system with measures that might provide incremental improvements in value. But first things first.
]]>